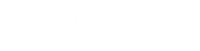Use the 5 A's to Assess and Address Tobacco Use
When you integrate the brief, supportive 5 A's counseling intervention into your routine clinical practice, you and your team can motivate your patients or clients who use tobacco to consider or make a quit attempt and reinforce abstinence in those who have quit.
Counseling
Patients who use tobacco are more likely to make a quit attempt when they have your support.
Brief cessation counseling, particularly when combined with FDA-approved medications, is effective and improves quit rates.
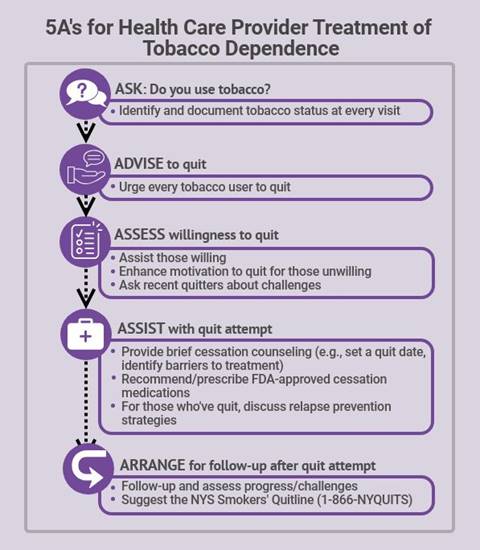
Use the 5 R's to Motivate Patients Unwilling to Quit
Patients not ready to make a quit attempt may respond to a brief, motivational intervention. Use the 5 R's to motivate patients to consider a quit attempt.
For More Information
- Identifying and Treating Patients Who Use Tobacco – Action Steps for Clinicians (Centers for Disease Control and Prevention): information on the 5 A's and 5 R's counseling models and FDA-approved cessation medications
- Quick Reference Guide for Clinicians - Treating Tobacco Use and Dependence (U.S. Department of Health and Human Services): detailed information on the 5 A's, 5 R's, motivational interviewing strategies, pharmacotherapy, relapse, and relapse prevention
- Protocol for Identifying and Treating Patients Who Use Tobacco (U.S. Department of Health and Human Services)
Reference
- Fiore MC, Jaén CR, Baker TB, et al. Treating Tobacco Use and Dependence: 2008 Update—Clinical Practice Guidelines. Rockville (MD): U.S. Department of Health and Human Services, Public Health Service, Agency for Healthcare Research and Quality, 2008.